 
Isolated tibial stress fractures usually heal very well and have little impact on the ability to return to full activity. During the recovery period the patient can take increased calcium and vitamin D through diet or supplements. RecoveryĬomplete recovery of uncomplicated stress fractures is typically around 12 weeks. Intermittent use of crutches may help with the transition. In many tibia fractures, the smaller bone in the lower leg (fibula) is broken as well. Motor vehicle collisions, for example, are a common cause of tibial shaft fractures. It typically takes a major force to cause this type of broken leg. The patient may resume weight-bearing on the injured leg once they are able to walk without pain. A tibial shaft fracture occurs along the length of the bone, below the knee and above the ankle. In some cases, a short period of non-weight-bearing may be necessary with the affected leg being splinted. Initial treatment includes rest and stabilization. When confirmatory imaging is required, such as an athlete who will be performing vigorous rehabilitation, magnetic resonance imaging (MRI), or a bone scan can show the presence of the stress fracture at an earlier stage. Three to four weeks after the diagnosis, an x-ray will typically show findings of a healing fracture. In most cases a positive x-ray is not necessary to begin treatment. Confirmation of a tibial stress fracture on initial x-rays occurs in less than half of the cases. 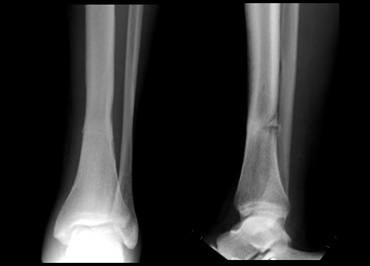
This article looks in detail at types of tibial fractures, along with the symptoms. Symptoms such as pain and discomfort precede signs of a fracture on x-ray. Fractures can be treated by a medical professional, and at-home exercises can speed up a person’s recovery. Sensitivity to vibration and the inability to hop on the affected leg without pain are also suggestive of a tibial stress fracture. Some swelling and localized tenderness of the bone will often be present. Physical exam will show pain that is specific to one area of the lower leg (tibia). Patient with lower bone density (osteoporosis) due to aging, vitamin D deficiency, or low body weight are at higher risk for developing a tibial stress fracture. The most common site of tibial stress fracture is the shaft of the bone, though they may also occur on the inside bony prominence of the ankle (medial malleolus) or the upper portion of the tibia that involves the knee joint (tibial plateau). In athletes, an increase in training intensity or volume precedes the onset of pain. The pain will gradually increase over the course of weeks and can reach the point that pain is felt at rest. However, a tibial stress fracture can often be distinguished by more localized pain and a longer course of onset. Initially symptoms commonly resemble shin splints (medial tibial stress syndrome). Most tibial stress fractures respond well to rest and a complete return to full activity is generally expected. osteoporosis) are at higher risk of developing a tibial stress fracture. Tibial stress fractures are distinguished from shin splints as the pain is more localized and more intense. It is caused by increased repetitive loading through the tibia – commonly in runners as a result of overtraining. Therefore, high-risk stress fractures require aggressive treatment.A tibial stress fracture is a localized fracture of the lower leg bone (tibia) at the microscopic level – it often cannot be seen on plain x-rays. Tensile forces and the relative avascularity at the site of a stress-induced fracture often lead to poor healing. Specific sites for this type of stress fracture are the femoral neck (tension side), the patella, the anterior cortex of the tibia, the medial malleolus, the talus, the tarsal navicular, the fifth metatarsal, and the great toe sesamoids. This topic review will discuss stress fractures of the tibia and fibula in adults and children. A subset of stress fractures can present a high risk for progression to complete fracture, delayed union, or nonunion. Most stress fractures are uncomplicated and can be managed by rest and restriction from the precipitating activity. The diagnosis is primarily clinical, but imaging modalities such as plain radiography, scintigraphy, computed tomography, and magnetic resonance imaging may provide confirmation. The classic presentation is a patient who experiences the insidious onset of pain after an abrupt increase in the duration or intensity of exercise. Intrinsic factors, such as hormonal imbalances, may also contribute to the onset of stress fractures, especially in women. The pathogenesis is multifactorial and usually involves repetitive submaximal stresses. Stress fractures are common overuse injuries seen in athletes and military recruits. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
